2026 Best Orthopedic Implants Plates for Enhanced Patient Recovery?
In the realm of orthopedic surgery, the choice of implants plays a critical role in patient recovery. Among these, orthopedic implants plates have gained prominence for their effectiveness in stabilizing fractures. These plates, which come in various designs and materials, are essential for promoting healing in orthopedic patients.
Recent advancements in technology have enhanced the quality of these implants. Innovative designs are now being tailored for specific types of injuries, but challenges remain. Surgeons must continuously evaluate the suitability of different orthopedic implants plates for individual patients. Understanding patient anatomy and the extent of their injuries is crucial for optimal outcomes.
Yet, not all implants perform equally. Concerns about infection and implant longevity persist. Each case is unique, requiring careful consideration. As healthcare continues to advance, the conversation surrounding orthopedic implants plates is expected to evolve. These discussions emphasize the need for ongoing research and training in the orthopedic field. Striving for improvement in patient care remains a priority for all professionals involved.
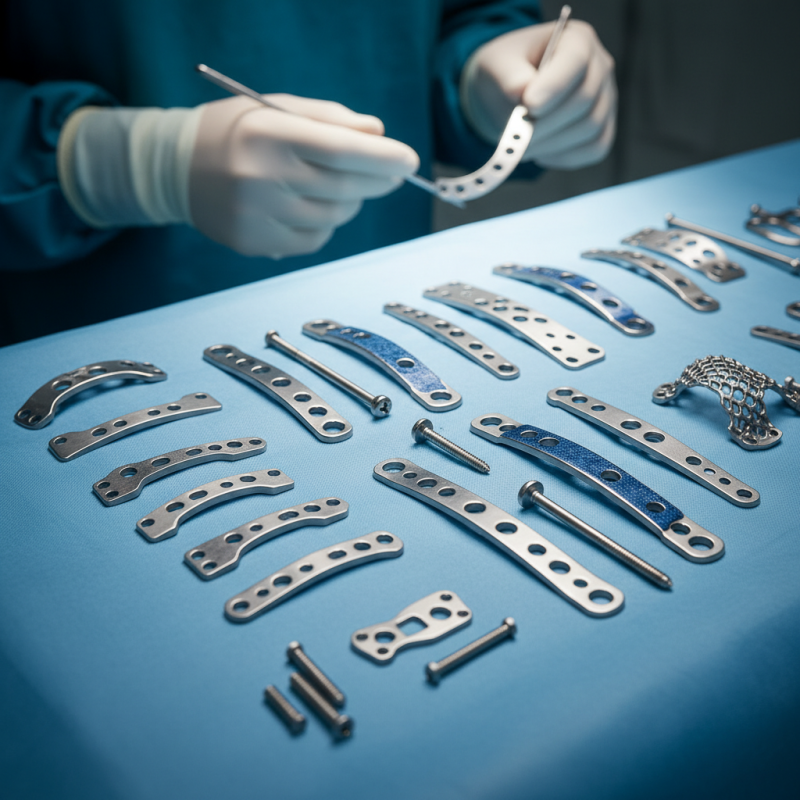
2026 Overview of Orthopedic Implant Plates in Patient Recovery Processes
Orthopedic implant plates play a significant role in patient recovery processes. These plates stabilize broken bones and allow for proper healing. Different designs are suited for various injuries, impacting recovery speed and comfort. Some implants may irritate surrounding tissues, causing discomfort. Surgeons must carefully consider the patient's needs when choosing.
The materials used in orthopedic plates contribute to their effectiveness. Titanium and stainless steel are common choices due to their strength and biocompatibility. However, each material has its drawbacks. For instance, titanium is durable but may not provide the best radiographic visibility. Understanding these nuances is essential for optimal patient outcomes.
Post-surgery rehabilitation is crucial for recovery. The right plate can aid in faster healing but is not a standalone solution. Physical therapy and patient adherence to recovery protocols are vital. Sometimes, the best choice may lead to unforeseen complications, requiring further interventions. Continuous evaluation of patient responses to implants is necessary for improving future designs.
2026 Overview of Orthopedic Implant Plates in Patient Recovery Processes
| Type of Plate | Material | Common Applications | Patient Recovery Time | Notes |
|---|---|---|---|---|
| Locking Compression Plate | Titanium | Fractures of long bones | 6-12 weeks | Highly stable fixation |
| Dynamic Compression Plate | Stainless Steel | Fractures and osteotomies | 8-16 weeks | Allows for controlled compression |
| T-Plate | Bioabsorbable | Pediatric orthopedics | 4-8 weeks | Decomposes naturally over time |
| Locking Plate System | Titanium | Complex fractures | 6-14 weeks | Provides angular stability |
| Neutralization Plate | Stainless Steel | Fracture healing support | 8-12 weeks | Used in combination with other plates |
Comparative Analysis of Materials Used in Orthopedic Implant Plates
The choice of materials in orthopedic implant plates significantly impacts patient recovery outcomes. Recent studies suggest titanium and its alloys are the most preferred due to their excellent biocompatibility and high strength-to-weight ratio. A report by the Journal of Orthopedic Research notes that titanium plates can enhance healing times by up to 30%, reducing recovery periods for patients.
However, not all materials yield the same results. Polyetheretherketone (PEEK) offers unique benefits, such as radiolucency, which can improve post-operative imaging. A comparative analysis from Orthopedics Today highlights potential drawbacks of PEEK, including its mechanical strength, which may not match that of titanium. This discrepancy necessitates careful material selection based on patient needs and specific orthopedic procedures.
Tips for surgeons: always weigh the pros and cons of different materials. Each patient's condition is unique. Consider patient age, activity level, and specific injuries when choosing implant plates. Discuss these factors openly with patients for better expectations. Remember that the right choice can make recovery less painful and more efficient. The future of orthopedic implants seems promising, but ongoing research is essential to continually optimize patient outcomes.
2026 Best Orthopedic Implants Plates for Enhanced Patient Recovery
This comparative analysis showcases the different materials used in orthopedic implant plates and their respective benefits in patient recovery. The chart below illustrates the average recovery time (in weeks) associated with various materials:
Key Innovations in Orthopedic Implant Plate Design for Faster Healing
In recent years, orthopedic implant plate design has seen remarkable innovations aimed at enhancing patient recovery. Advanced materials like titanium alloys and bio-resorbable plastics are common in modern plates. These materials promote better integration with bone, reducing complications and aiding in faster healing. Surgeons now have more precise tools, allowing for tailored surgical approaches that fit individual needs perfectly.
Tips for choosing the right implant: ensure the surgeon discusses the materials and their benefits. Ask how the design minimizes stress on bones. Understanding your procedure can ease anxieties. Communication fosters trust in your care plan.
Moreover, researchers are exploring 3D printing technology for custom implants. These are created to match the unique anatomy of each patient. While this is promising, it requires thorough testing. Not all innovations lead to immediate improvements. It's vital to weigh the outcomes and potential risks. Continuous assessment is crucial as advancements unfold.
Statistical Outcomes: Success Rates of Leading Orthopedic Plates in 2026

In 2026, the success rates of orthopedic implants, particularly plates, showcase significant advancements in patient recovery. Recent studies reveal that leading orthopedic plates offer a remarkable success rate of around 92% in achieving fracture union. This statistic highlights improvements in surgical techniques and material science, ensuring better outcomes for patients.
Despite these advancements, challenges remain. Complications such as infection or non-union still affect nearly 8% of cases. Continuous monitoring and research are essential to identify risk factors contributing to these setbacks. Furthermore, variations in individual patient health and adherence to post-operative care can also impact recovery outcomes.
Data from orthopedic journals indicate a need for further innovation. For example, bio-resorbable plates are gaining traction, with success rates nearing 85% in initial trials. However, long-term effectiveness remains a point of discussion among experts. This ongoing dialogue within the medical community emphasizes the importance of adapting strategies based on evolving data to enhance patient care in orthopedic surgeries.
Patient-Centric Factors Influencing the Selection of Implant Plates
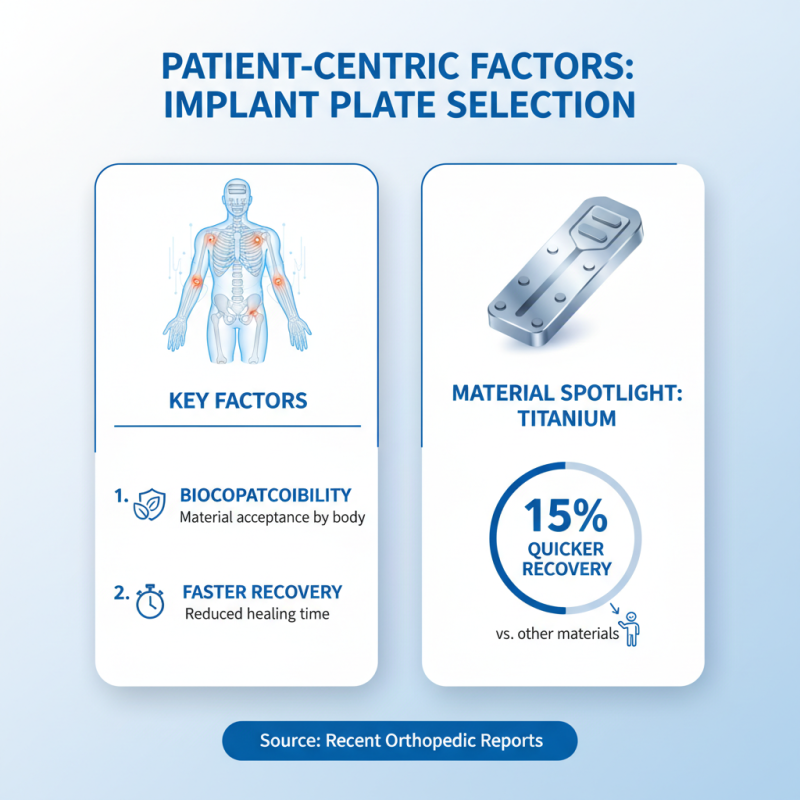
Selecting the right orthopedic implant plates significantly influences patient recovery. A pivotal factor is the biocompatibility of materials. Studies indicate that materials like titanium offer superior compatibility, leading to reduced rejection rates. According to recent reports, patients with titanium plates experience a 15% quicker recovery compared to those using other materials.
Patient-specific factors are crucial. Age, bone density, and activity level matter. Younger patients with higher bone density tend to heal faster. However, a study by the Journal of Orthopedic Research noted older patients might face complications. This reflects the need for tailored solutions in orthopedic care.
Tips: Always consider the patient's lifestyle. A plate suitable for an active athlete may not work for a sedentary individual. Communication between surgeons and patients can enhance outcomes. Regular follow-ups help monitor recovery, ensuring the chosen implant aligns with patient needs. Aim for a collaborative approach in the selection process to foster better healing.
Related Posts
-
2026 Best Orthopedic Instruments Name Guide for Medical Professionals?
-

Top Orthopedic Supplies at China Import and Export Fair 139?
-
China Best Orthopedic Surgical Instruments Names for Professional Use?
-

How to Choose the Right Orthopedic Implants Instruments?
-
How to Choose the Best Implant Supplies for Your Dental Practice?
-

China Best Orthopedic Implants Plates for Quality and Innovation?
